Shutterstock.com
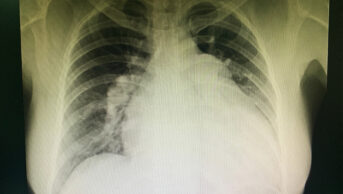
Hundreds more patients admitted to hospital with heart failure are surviving because of improvements in care, an independent audit commissioned by the NHS has found.
The National Heart Failure Audit was established in 2007 to monitor the care and treatment of patients with acute heart failure in England and Wales.
The latest report, published on 10 August 2017 and based on an analysis of 66,695 admissions to English and Welsh hospitals between April 2015 and March 2016, where the patients’ main diagnosis was heart failure, found a mortality rate of 8.9%. This compared with a mortality rate of 9.6% for the same period in 2014–2015, meaning that around 500 more people with heart failure were saved in 2015–2016. However, there were large variations in mortality rates between hospitals. Patients admitted to cardiology wards and treated by heart failure specialists fared better.
During hospital admission, more than 90% of patients were recorded as having had an up-to-date echocardiogram, and rates were higher for those admitted to cardiology (96%) rather than general medical (85%) wards. Specialist input, irrespective of the place of admission, was also associated with higher rates (95%) of echocardiography.
Sir Bruce Keogh, national medical director at NHS England, said: “We recognise that there is scope for even more improvement but the progress highlighted today will be a spur for us to do even more to improve care and survival rates.”
The report shows that prescription rates for all three key disease-modifying medications (angiotensin converting enzyme inhibitors (ACEI), beta-blockers (BB) and mineralocorticoid (aldosterone) receptor antagonist (MRA)) for patients with a reduced left ventricular ejection fraction (HF-REF) have increased from 35% to 53% for those admitted to cardiology wards over the last six years. Irrespective of the place of admission, 47% of patients with HF-REF seen by a member of the specialist heart failure team as an inpatient, were prescribed all three disease-modifying drugs, compared with 45% in the previous year.
Had the patients identified as having HF-REF, who left hospital on none of the three disease-modifying drugs, been prescribed all three, at least an additional 212 patients would likely have been alive at the time of the audit, the report says.
“This year’s report shows modest but important improvements which are to be celebrated. But an 8.9% inpatient mortality cannot be accepted and requires urgent attention,” it emphasises.
The latest National Heart Failure Audit is the largest ever, using data from 82% of all heart failure admissions in England and 77% of those in Wales.