
Shutterstock.com
When you start your career as a pharmacist you will come across many situations where you give advice on prescribing options, particularly when working with junior doctors. In such situations you realise quickly that you make the decisions about what to prescribe and when — but then have to ask the prescriber to sign the prescription and take over responsibility for your choices. This is frustrating. By becoming an independent prescriber you can resolve this problem.
Pharmacists can attain two types of prescribing qualification: independent and supplementary. Independent prescribers, or non-medical prescribers (NMPs), are in a position to give patients timely access to medicines and are ideally placed to optimise and individualise treatment. The NMP takes responsibility for the clinical assessment of the patient, including establishing a diagnosis and prescribing the necessary medicines. Supplementary prescribing, on the other hand, is a voluntary partnership between a doctor or dentist and a supplementary prescriber, who can prescribe medicines within an agreed patient-specific clinical management plan with the patient’s agreement[1].
Pharmacists, nurses, optometrists, physiotherapists and podiatrists can all train to become independent prescribers. Optometrists, physiotherapists and podiatrists can only prescribe within their own specialty, whereas pharmacists and nurses are able to prescribe any medicine for any medical condition within their competence.
The expanding role of the pharmacist independent prescriber
Pharmacist NMPs in hospital often deal with medication reviews and medicine reconciliations, which ensure that an accurate list of current medicines is compiled for patients admitted to hospital, and help to optimise treatment processes. In community pharmacy, NMPs are usually involved in running minor ailment services or visiting care homes.
However, because of the level of independence afforded to an NMP, pharmacist NMPs working within a multidisciplinary team can be involved in any task that is necessary to deliver the service without being concerned about whether it falls strictly within their job description. This is useful because organisations have started to consider alternative models of care to help patients optimise their medicines use. For example, in primary care, some GP practices have nurse-led asthma clinics and pharmacist-led care home medicine review services. In secondary care, anticoagulation clinics are overseen by consultants but may be managed by pharmacist or nurse NMPs.
Therefore, acquiring the NMP qualification can give pharmacists a wide range of opportunities to expand their roles, if they think creatively. For example, I run an infusion clinic, which traditionally is done by nurses. I also manage the prescribing of biologics for dermatology and inflammatory bowel disease patients. I regularly assess patients for their response to the medicines, supported by an innovative therapeutic drug monitoring service.
Qualifying and developing
All non-medical prescribing is underpinned by legislation and regulatory standards. The National Prescribing Centre competency framework1, which is currently under review, stipulates that aspiring NMPs need to be experienced practitioners before they can begin the education programme necessary to become prescribers. It will depend on the organisation you work for what prior experience is required to be eligible for the prescribing course. However, in hospital practice, a candidate must usually be working at the “Agenda for change” NHS pay band 7 or above. Most employers would also expect a candidate to have some level of specialisation.
Usually an employer will fund some or all of the course fees because having a qualified NMP delivering care benefits the service provided.
Many universities offer the course with varied curricula and the programme usually lasts for six months. In most courses, nurses and pharmacists will study together, which immediately helps students to break down barriers and develop an understanding for each other’s roles. The current course does not teach diagnosis in depth, so it is up to the practitioners to ensure that their diagnostic skills are appropriate to their practice and demonstrate competency. This may involve additional training in specific physical examination skills or interpretation of electrocardiograms or biochemical tests.
The single competency framework provides an outline of common prescribing competencies that, if acquired and maintained, can help all prescribers to become and remain effective prescribers in their area of practice.
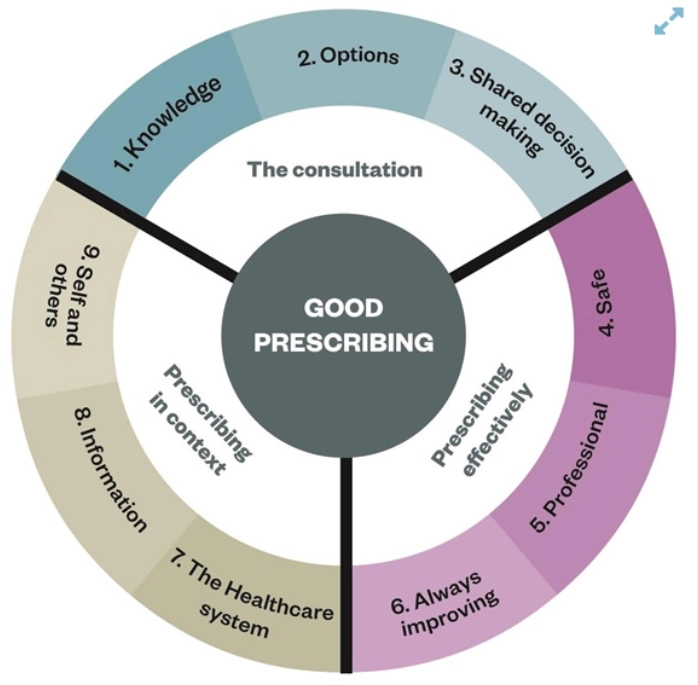
Prescribing competency framework
The competency framework from the National Prescribing Centre sets out what good prescribing looks like
The competency framework (see above) sets out what good prescribing looks like. There are three domains, each containing three dimensions of competency. Within each of the nine competency dimensions there are statements that describe the activity or outcomes prescribers should be able to demonstrate. For example, the first statement in “the consultation” under “knowledge” reads: “understands the conditions being treated, their natural progress and how to assess their severity”.
Once qualified, all NMPs must record their qualification with their professional regulator. Independent prescribers have a responsibility to remain up to date with the knowledge and skills that enable them to prescribe competently and safely. This means that they must complete appropriate continuous professional development and this can effectively be achieved by working in a multidisciplinary team. In community, this may mean NMPs must be affiliated with a GP practice or another multidisciplinary forum for support and professional development.
Starting off as a surgical pharmacist I was not clear how the qualification could benefit my practice. However, I developed a general scope of practice for pharmacists working on wards endorsed by the trust. From there I found many more opportunities to develop my role in unexpected directions, providing a satisfying and enriching career progression.
References
- A single competency framework for all prescribers. National Prescribing Centre, May 2012. http://www.npc.co.uk/improving_safety/improving_quality/resources/single_comp_framework_v2.pdf


