Nephron / Wikimedia Commons
In this article you will learn:
- How to assess warts and verrucas
- Red flag symptoms for skin lesions requiring specialist advice
- The different wart treatments available
Warts are common viral skin infections, affecting around 7–12% of the population at any one time, and are more common in children[1]
. They are caused by the human papilloma virus (HPV), of which there are over 150 genotypically different types; the most common are HPVs 1, 2, 4, 27 and 57, and HPVs 3 and 10 for plane (flat) warts.
HPV infects the keratinocytes, the most dominant cell type in the epidermis, which results in development of epidermal thickening and hyperkeratinisation. HPV infection is acquired from direct contact, which may be person-to-person or from the environment (e.g. showers and swimming pools; skin penetration increases if the skin is broken or wet)[2]
.
Studies suggest that the bovine papilloma virus (which is related) can retain infectivity for months and possibly years, and the same may be true for HPV[3]
.
Verrucas are plantar warts, located on the sole of the foot[4],[5]
. Someone with a plantar wart should use waterproof plasters in communal bathing areas; verruca socks are also available.
This article will not discuss anogenital warts or seborrhoeic (keratoses) warts.
Assessment
When clinically assessing skin lesions, the following steps are useful to aid diagnosis[6],[7]
:
- Inspect the patient. Where on the body are the lesions? How many lesions are there? If there are multiple lesions, do they follow a pattern or are they on a specific area?
- Describe the lesions. What is the largest diameter of lesion? Is there colour? Are there any secondary changes (e.g. lichenification, crusting, excoriation (scratch marks), ulceration, erosion, fissure (thin crack), hypertrophy (increase in skin) or granuloma?) Is there a clear defined border? Is it regular?
- Palpate the lesion. Feel the surface, consistency, mobility, tenderness and temperature (use gloves to prevent infection).
- Check the patient’s overall health. Examine the nails, scalp, hair and mucous membranes. Is there any lymphadenopathy? Does the patient have a temperature?
Any pigmented lesions should be checked for red flags suggestive of melanoma. These include: asymmetry (lack of mirror image lesion in any of the four quadrants of the body); irregular border; two or more colours in the lesion; diameter of more than 7mm. Patients presenting with any of these symptoms should be referred to a dermatologist for further assessment (e.g. biopsy and histological studies).
Cutaneous warts are generally diagnosed on appearance. The characteristic appearance of different types of warts are as follows:
- Common warts are firm and raised with rough edges like a cauliflower;
- Plane warts are round, flat-topped and yellow, and they are commonly seen on the back of hands;
- Filiform warts are long, finger-like warts common on the face and neck;
- Palmar and plantar warts grow on palms (palmar) and soles of feet (plantar). Often seen with thrombosed capillaries, which appear as a central black dot (these do not appear in corns and calluses);
- Periungual warts occur around fingernails and toenails, and appear as thickened, cauliflower-like skin;
- Mosaic warts are multiple palmar or plantar warts that coalesce on hands or feet.
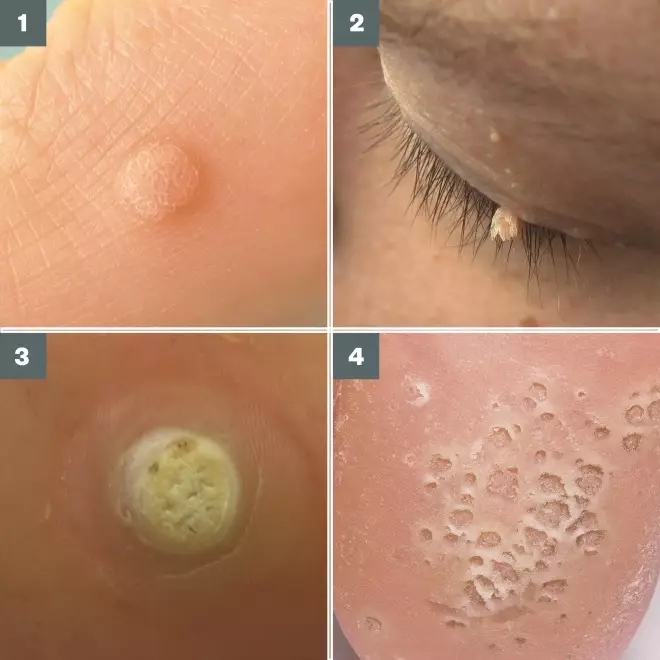
Photoguide of different types of wart
Source: L-R: BSIP SA/Alamy / Wikimedia Commons / James Heilman/Wkimedia Commons / Alamy
1) Plane wart; these are most common on the backs of hands and are round and flat-topped
2) Filiform wart; long, finger-like warts that appear on the face and neck
3) Plantar wart; these can be differentiated from corns by the presence of black dots (seen top centre), which are thrombosed capillaries.
4) Mosaic warts; these are groups of palmar or plantar warts.
The presentation can be similar to other lesions. Possible differential diagnoses for warts on the hands or feet include[5]
: actinic keratosis; seborrheic keratosis; knuckle pads; squamous cell carcinoma; lichen planus; corns or calluses; and malignant melanoma.
If the diagnosis is in doubt, paring down a wart with a file will result in pinpoint bleeding from thrombosed capillaries[5]
. Paring should be performed with caution, as the bleeding contains active viral DNA that can infect the clinician or further the spread of infection[4]
. If in doubt, the patient should be referred to a clinician specialising in dermatology to confirm diagnosis. Patients should also be referred if they have a facial wart or extensive areas of the skin are affected (usually mosaic warts on the hands and feet).
Warts can last longer in patients who are immunocompromised, especially those with cell-mediated immunodeficiency. In patients with severely impaired immune function (e.g. patients treated with immunosuppressants after organ or bone marrow transplant), warts may be large, extensive and resistant to treatment. Warts can also be a presenting complaint of patients with undiagnosed conditions such as HIV, lymphoma and CD4 lymphocytopenia. All patients with warts who are immunocompromised should be referred to a dermatologist.
HPV infection is associated with squamous cell carcinoma and pre-malignancy. The likelihood of squamous cell carcinoma is increased in mild immunodeficiency and carriers of certain HPV types. HPV types 5 and 8 are also associated with epidermodysplasia verruciformis, an extremely rare skin disorder that results in the growth of scaly macules and papules.
Treatment
No treatment is required in most cases, especially if the warts cause no functional impairment. Most warts will resolve spontaneously within two years, although some cases can take five to ten years to resolve. Treatment should be considered when the wart is uncomfortable, function is impaired or if the warts affect appearance (e.g. warts on the face).
Most warts and verrucae can be treated in primary care. In some cases, referral to a hospital specialist may be necessary (e.g. if persistent warts show a poor response to treatment), however local policies may restrict treatment to symptomatic warts only[4]
.
Treatment options include salicylic acid, often in combination with lactic acid, formaldehyde, glutaraldehyde and cryotherapy.
Topical salicylic acid (15–50% w/w), applied to the wart daily for 12 weeks, is the treatment of choice for adults and older children. Its exact mechanism of action is not known but it acts as a keratolytic, resulting in the removal of epidermal cells infected by HPV. It is also effective at removing corns and calluses.
A Cochrane review of treatments found the chance of clearance of warts with salicylic acid was 1.56 times greater compared with placebo. Removal was most effective on hands (relative risk 2.67) compared with feet (relative risk 1.29)[8]
.
Salicylic acid preparations are available in a range of treatments, including gels, paints, solutions and ointments, and they often also include lactic acid; in the UK, these are available over the counter. Gel treatments may also contain colophony, which may cause an allergic reaction in some patients[9]
.
Salicylic acid should not be applied to warts on the face, intertriginous areas (where skin rubs together, such as the axilla), anogenital warts, moles or birthmarks, warts with hair or red edges, or to open lesions or broken skin[4]
. When using salicylic acid, patients should be advised to protect the surrounding skin to avoid irritation; this can be done by coating the area with soft paraffin or by using plasters.
Salicylic acid is not recommended to treat plantar warts in patients with diabetes, as these patients often have peripheral neuropathy and poor circulation, leading to poor wound healing[4]
. The NHS states that salicylic acid can be used to treat warts in pregnancy but only on a small area for a limited period of time.
Formaldehyde and glutaraldehyde are applied in a similar way to salicylic acid. Glutaraldehyde can stain the skin brown, and should be discontinued if skin irritation is severe.
Patients using over-the-counter treatments can be advised to debride the surface of the wart gently with a file (e.g. emery board) or pumice stone once weekly. However, this should be done carefully as there is a risk of further spread of the infectious material. Patients should also soak the wart for five minutes before treatment to soften it.
Cryotherapy with liquid nitrogen is suitable for adults and older children who are able to tolerate it. It causes rapid cooling of cells, causing ice crystals to form outside of cells, and disrupts membranes. When thawing occurs, extracellular fluid becomes hypertonic, with the rapid flow of water into cells causing cell death[10]
.
Treatment usually involves exposure to liquid nitrogen every two weeks for three to four months. A session takes between 5–15 minutes, and may be painful. After treatment a blister forms, followed by a scab, which falls off around a week later. Cryotherapy can cause local irritation to unaffected skin[3]
. Other side effects include scarring (rare), hyperpigmentation, which usually improves with time but may be permanent, and paraesthesia caused by freezing a superficial nerve cell; this will return to normal after two to three months.
There are no defined age limits for cryotherapy. It can be used to treat younger children, although it is not usually recommended. Each treatment should be no longer than five to ten seconds in these patients.
Cryotherapy is not recommended for areas with a tendon, as aggressive treatment can cause tendon damage. Onychodystrophy (malformation of the nails) may occur if periungual warts are treated with cryotherapy[4]
.
Silver nitrate pencils are also available to treat cutaneous warts; however, there is no good evidence that this is effective[3]
.
The Cochrane review also found no evidence that using duct tape to treat warts was more effective than placebo[8]
.
Sam Akram is a senior lecturer at Anglia Ruskin University and GP practice-based pharmacist. Hadar Zaman is a lecturer at University of Bradford and community pharmacist.
References
[1] Lynch MD, Cliffe J & Morris-Jones R. Management of cutaneous viral warts. BMJ 2014;348:g3339. doi:10.1136/bmj.g3339.
[2] Sterling JC. Virus infections. In: Burns. Breathnach S, Cox N & Griffiths C. (Eds.) Rook’s textbook of dermatology. 8th ed . Chichester: Wiley-Blackwell; 2010. 33.1–33.81.
[3] Sterling J, Gibbs S, Hussain S et al. British Association of Dermatologists’ guidelines for the management of cutaneous warts 2014. Br J Dermatol 2014;171(4):696–712.
[4] National Institute for Health and Care Excellence. Clinical Knowledge Summaries. (2014). Warts and Verrucae. Available at: http://cks.nice.org.uk/warts-and-verrucae#!references (accessed May 2015).
[5] Dinulos JGH. Warts. Available at: http://www.merckmanuals.com/professional/dermatologic-disorders/viral-skin-diseases/warts (accessed May 2015).
[6] Macleod J.Macleod’s Clinical Examination. 12th ed. London: Churchill Livingstone; 2009.
[7] British Association of Dermatologists. Medical Students Edition. 2015. Software application.
[8] Kwok CS, Gibbs S, Bennett C et al. Topical treatments for cutaneous warts. Cochrane Datab Syst Rev. doi:10.1002/14651858.CD001781.pub3.
[9] Royal Pharmaceutical Society and British Medical Association. British National Formulary 69. London: RPS 2015.
[10] Nguygen NV & Burkhart CG. Cryosurgical treatment of warts: dimethyl ether and propane versus liquid nitrogen — case report and review of the literature. J Drugs Dermatol 2011;10:1174–117.